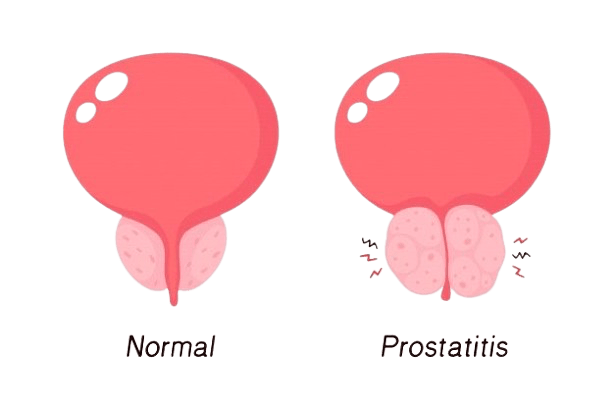
Introduction
Stress doesn’t just live in the mind—it leaves an imprint on the body. For many men, chronic stress, poor posture, and shallow breathing can subtly contribute to pelvic tension and urinary issues. While standard medical care often focuses on the prostate itself, deeper contributors such as nervous system regulation and pelvic floor health are often overlooked. Understanding the relationship between stress, movement, and urinary function offers a more complete path to relief—and lasting wellness.
Men with urinary urgency, retention, or discomfort may benefit from daily habits that calm the nervous system, address pelvic tension, and support natural function. Prostate and bladder neck function are influenced by a network of muscles, nerves, and connective tissue, which are sensitive to stress, posture, and movement.
Chronic stress, shallow breathing, and prolonged sitting can increase pelvic tension, impacting the urethra and bladder signaling. Medical treatments often reduce prostate size or muscle tone pharmacologically but may overlook how pelvic floor and nervous system health affect symptoms.
Yoga and breathwork can support pelvic floor relaxation, stimulate blood flow, and regulate the nervous system. Studies show yoga can improve urinary symptoms in men with benign prostatic hyperplasia (BPH), attributed to pelvic muscle relaxation, enhanced circulation, and reduced stress. Breath-focused techniques can reduce pelvic discomfort and improve quality of life.

Recommended Practices
Diaphragmatic (deep belly) breathing for five minutes: Inhale through the nose, letting the belly rise, then exhale slowly with relaxation of the pelvic floor.
Reclining Bound Angle Pose (Supta Baddha Konasana): Opens groin and inner thighs, encouraging pelvic floor release.
Deep Squat (Malasana): Decompresses pelvic floor and bladder neck.
Bridge Pose (Setu Bandhasana): Strengthens glutes, reduces pelvic tension.
Legs Up the Wall (Viparita Karani): Relieves pelvic congestion, calms the nervous system.
Alternate nostril breathing (Nadi Shodhana): Balances autonomic functions.
Humming bee breath (Bhramari): Soothes pelvic nerves, activates vagal calming.
Clinical research suggests consistent practice of these techniques can help men experiencing urinary hesitancy, weak stream, frequent or urgent urination, and incomplete bladder emptying, as well as those with BPH or chronic pelvic discomfort.
Consistency is key to progressive pelvic relaxation and improved urinary function.
Conclusion
Urinary symptoms like urgency, weak stream, or incomplete emptying don’t always begin with the prostate—and they don’t always end with medication. Gentle, consistent practices that release pelvic tension, calm the nervous system, and restore breath-body connection can support meaningful change. Through mindful movement and breath, men can take a more active, natural role in their own healing. The body has the ability to rebalance—sometimes, it just needs a little help remembering how.

Explore More at Rise & Inspire archive. | Motivational Blogs |
Categories: Astrology & Numerology | Daily Prompts | Law | Motivational Blogs | Motivational Quotes | Others | Personal Development | Tech Insights | Wake-Up Calls
🌐 Home | Blog | About Us | Contact| Resources
📱 Follow us: @RiseNinspireHub
© 2025 Rise&Inspire. All Rights Reserved.
Word Count:481