Learn how high and low blood sugar levels affect your body, from fatigue and thirst to vision problems and heart risks. Discover symptoms, management tips, and when to seek medical help to keep your blood sugar balanced and your health on track.
How High and Low Blood Sugar Levels Affect Your Body
Maintaining balanced blood sugar levels is essential for overall health, especially for individuals managing conditions like diabetes. When blood sugar levels swing too high (hyperglycemia) or too low (hypoglycemia), they can impact your body in various ways, affecting both your entire system and specific areas. Understanding these effects can help you recognise symptoms early and take action to manage your health effectively. In this blog post, we’ll break down how high and low blood sugar levels affect your body, as illustrated in the infographic below, and provide tips for keeping your levels in check.
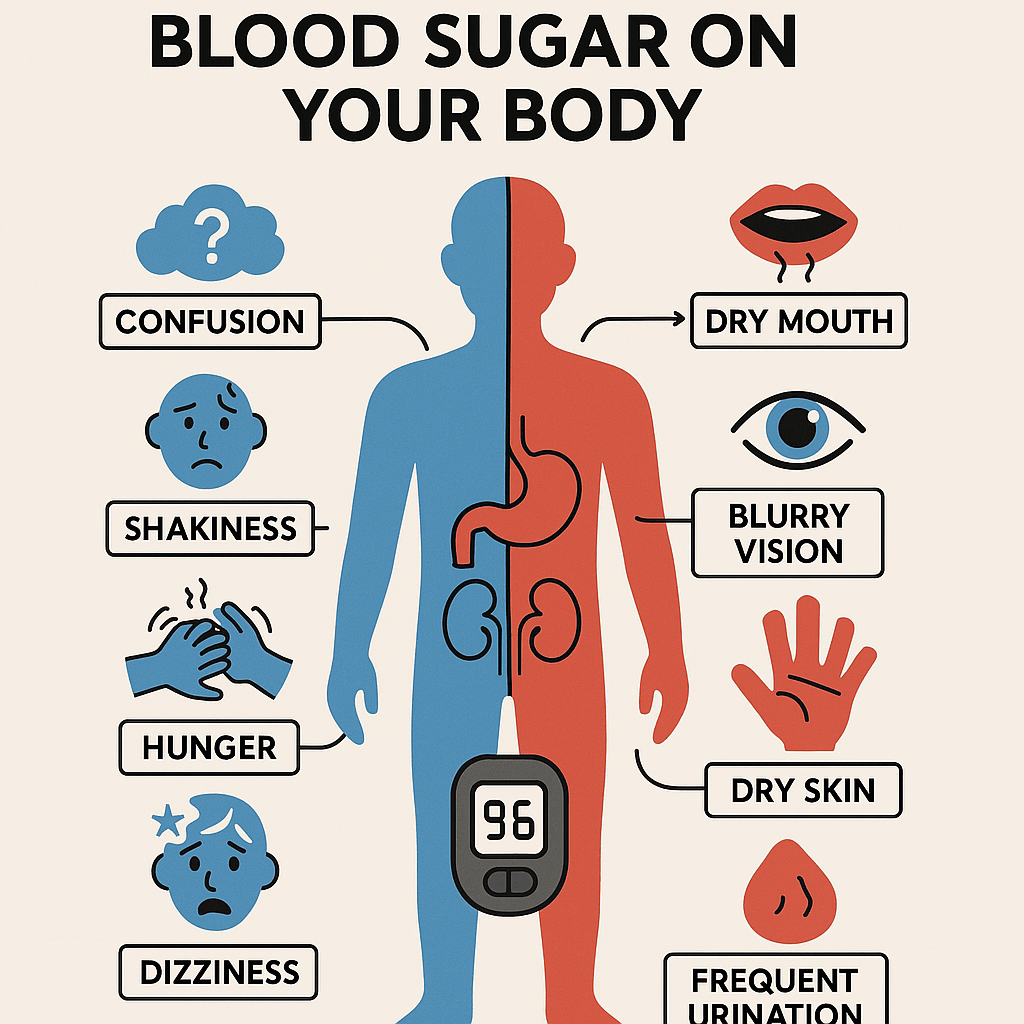
The Impact of High and Low Blood Sugar Levels
Entire Body Effects
Blood sugar imbalances can affect your whole body, leading to symptoms that impact your energy, mood, and overall functioning.
Fatigue (High/Low): Both high and low blood sugar levels can leave you feeling exhausted. High blood sugar (hyperglycemia) causes fatigue because your cells aren’t getting the glucose they need for energy due to insulin resistance or deficiency. Low blood sugar (hypoglycemia) deprives your body of its primary fuel source, leading to tiredness and weakness.
Sweating and Shakiness (Low): When blood sugar drops too low, your body releases stress hormones like adrenaline to signal the need for glucose. This can cause sweating, trembling, and a jittery feeling as your body tries to correct the imbalance.
Specific Area Effects
Beyond whole-body symptoms, blood sugar fluctuations can target specific areas, causing a range of issues from head to toe.
Head and Brain
Low: Confusion
Hypoglycemia can impair brain function because glucose is the brain’s primary energy source. When levels drop, you may experience confusion, difficulty concentrating, or even irritability. In severe cases, it can lead to seizures or loss of consciousness.
High: Constant Thirst and Dry Mouth
Hyperglycemia causes your body to pull water from tissues to dilute the excess sugar in your blood, leading to dehydration. This results in persistent thirst and a dry mouth as your body signals the need for more fluids.
Eyes
High: Vision Problems
High blood sugar can cause swelling in the lens of the eye, leading to blurry vision. Over time, chronic hyperglycemia can damage blood vessels in the retina, increasing the risk of diabetic retinopathy, which can lead to vision loss if untreated.
Skin
High: Dry, Itchy, Cracked Skin
Dehydration from high blood sugar can dry out your skin, making it itchy and prone to cracking. Poor circulation and nerve damage (neuropathy) associated with chronic hyperglycemia can also worsen skin issues, increasing the risk of infections.
Stomach and Appetite
Low: Hunger
When blood sugar levels drop, your body signals a need for more fuel, often resulting in intense hunger or cravings for quick-energy foods like sugary snacks.
Low: Nausea and Dizziness
Hypoglycemia can also cause nausea and dizziness as your brain and body struggle with low glucose levels, disrupting normal digestion and balance.
High: Digestive Problems
Chronic high blood sugar can damage nerves that control digestion (a condition called gastroparesis), leading to issues like bloating, nausea, vomiting, or constipation.
Heart
Low: Heart Rhythm Problems
Severe hypoglycemia can stress the body, triggering irregular heartbeats (arrhythmias). This happens because low glucose levels affect the autonomic nervous system, which regulates heart rate.
Kidneys and Bladder
High: Frequent Urination
When blood sugar levels are high, your kidneys work overtime to filter out the excess glucose, which is excreted in urine. This process draws water out of your body, leading to frequent urination and further contributing to dehydration.
Managing Blood Sugar Levels: Tips for Balance
Understanding how blood sugar affects your body is the first step, but taking action to maintain balance is key to preventing these symptoms. Here are some practical tips to help you manage your blood sugar levels:
For Preventing High Blood Sugar (Hyperglycemia)
Monitor Regularly: Use a glucometer to check your blood sugar levels, especially if you have diabetes. Keeping track helps you identify patterns and adjust your habits.
Follow a Balanced Diet: Focus on low-glycemic foods like whole grains, vegetables, lean proteins, and healthy fats. Avoid sugary drinks and refined carbs that spike blood sugar.
Stay Hydrated: Drink plenty of water to help your kidneys flush out excess glucose and prevent dehydration.
Take Medications as Prescribed: If you’re on insulin or other diabetes medications, follow your doctor’s instructions carefully to keep levels in check.
Exercise Regularly: Physical activity helps your body use glucose more effectively and improves insulin sensitivity. Aim for at least 30 minutes of moderate exercise most days.
For Preventing Low Blood Sugar (Hypoglycemia)
Eat Regular Meals and Snacks: Don’t skip meals, especially if you’re on insulin or medications that lower blood sugar. Include a mix of carbs, protein, and fats to provide steady energy.
Carry a Quick Snack: Keep fast-acting carbs like glucose tablets, juice, or candy on hand in case you feel symptoms of low blood sugar.
Adjust Medications with Your Doctor: If you experience frequent lows, talk to your healthcare provider about adjusting your medication or insulin doses.
Monitor Before and After Exercise: Physical activity can lower blood sugar, so check your levels before and after working out, and eat a small snack if needed.
General Tips for Balance
Manage Stress: Stress can affect blood sugar levels by triggering hormones like cortisol. Practice relaxation techniques like deep breathing, meditation, or yoga.
Get Enough Sleep: Poor sleep can disrupt blood sugar regulation. Aim for 7–9 hours of quality sleep per night.
Work with Your Healthcare Team: Regularly consult with your doctor or a diabetes educator to create a personalised plan for managing your blood sugar.
When to Seek Medical Help
If you experience severe symptoms like persistent confusion, fainting, chest pain, or difficulty breathing, seek medical attention immediately. These could indicate a serious blood sugar imbalance or other complications that require urgent care.
The Bottom Line
High and low blood sugar levels can have a significant impact on your body, but with awareness and proactive management, you can minimise their effects. Pay attention to your body’s signals, monitor your levels, and adopt healthy habits to keep your blood sugar in a safe range. If you’re struggling to manage your levels or have concerns about your symptoms, don’t hesitate to reach out to your healthcare provider for guidance.
By staying informed and taking control, you can lead a healthier, more balanced life!
Explore additional inspiration from the blog’s archive. | Motivational Blogs
Categories: Astrology & Numerology | Daily Prompts | Law | Motivational Blogs | Motivational Quotes | Personal Development | Tech Insights | Wake-Up Calls
🌐 Home | Blog | About Us | Contact| Resources
📱 Follow us: @RiseNinspireHub
© 2025 Rise&Inspire. All Rights Reserved.
Word Count:1156