Rise & Inspire – Skin Health Awareness
Discover how diabetes can show up on your skin with signs like yellow patches, velvety spots, and itchy areas. Learn what these symptoms mean and how to take action for better health with Rise & Inspire.
Recognizing the Signs of Diabetes on Your Skin:
A Guide for Rise & Inspire Readers
Hello, Rise & Inspire community! Today, we’re looking into an important health topic that often goes unnoticed—how diabetes can manifest through changes in your skin. Your skin can be a window into your overall health, and for those living with or at risk of diabetes, certain signs can serve as early warning signals.
Let’s explore these signs, understand what they mean, and learn how to take action to prioritize your well-being.
Why Skin Changes Matter in Diabetes
Diabetes, a condition characterized by high blood sugar levels, affects millions of people worldwide. When blood sugar levels remain elevated over time, it can lead to various complications, including visible changes in the skin. These changes occur because high glucose levels can damage blood vessels, nerves, and tissues, impairing circulation and the skin’s ability to heal or function properly.
For many, skin symptoms can be one of the first indicators of diabetes—or a sign that the condition isn’t well-managed. Recognizing these signs early can prompt you to seek medical advice, potentially leading to a diagnosis or better management of the condition.
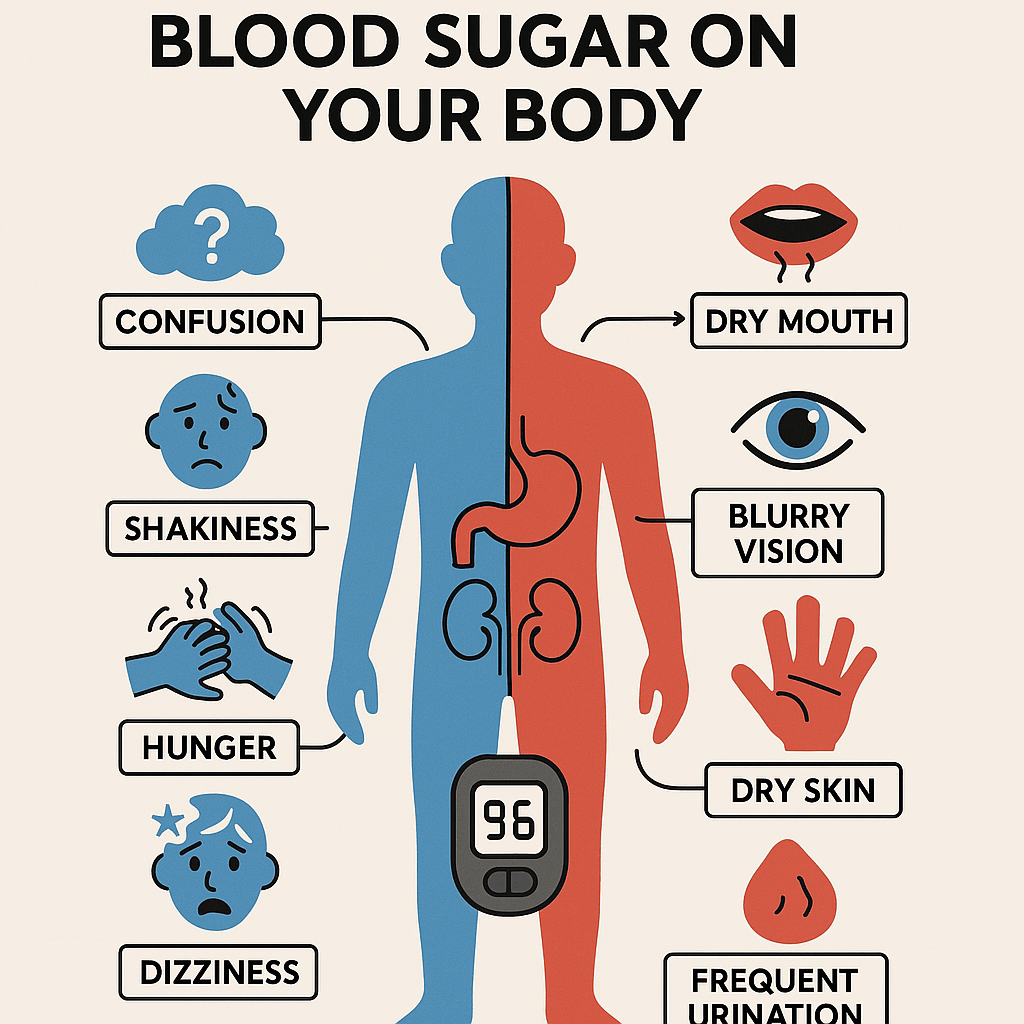
Let’s break down the key skin changes associated with diabetes, as highlighted in the image below.
Common Skin Signs of Diabetes
The following are six skin-related symptoms that could indicate diabetes. If you notice any of these in yourself or a loved one, it might be time to consult a healthcare professional.
1. Yellow or Brown Patches or Bumps
One condition linked to diabetes is eruptive xanthomatosis, which appears as small, yellowish or brownish bumps, often on the back, arms, or legs. These bumps are caused by high levels of triglycerides (a type of fat) in the blood, which can occur when diabetes is poorly controlled. They may be itchy or tender and are more common in people with type 1 diabetes.
2. Darker, Velvety Patches
A condition called acanthosis nigricans is often a sign of insulin resistance, a hallmark of type 2 diabetes. This appears as dark, velvety patches of skin, typically in areas with folds, such as the neck, armpits, or groin. The skin may feel thicker and have a different texture than the surrounding areas. While this condition can also occur in other hormonal disorders, it’s frequently associated with diabetes.
3. Hard-Thickened Areas
Digital sclerosis is a condition where the skin on the hands, fingers, or toes becomes thick, tight, and waxy. This is more common in people with type 1 diabetes and can make it difficult to move the fingers or toes. It often starts on the backs of the hands and can spread to other areas, like the arms or forehead. Managing blood sugar levels can help prevent or slow the progression of this condition.
4. Groups of Blisters
Diabetic blisters (bullosis diabeticorum) are rare but can occur in people with diabetes, especially those with nerve damage (neuropathy). These blisters often appear on the hands, feet, legs, or arms and look similar to burn blisters. They’re usually painless and heal on their own, but they can be a sign of poorly controlled diabetes. Keeping your skin clean and monitoring for infection is crucial if you develop these blisters.
5. Skin Spots or Depressions
Necrobiosis lipoidica is another skin condition tied to diabetes, though it’s less common. It starts as small, red spots that can grow into larger, shiny patches with a yellowish centre and a violet border. These spots often appear on the shins and can sometimes become itchy or painful. Over time, the skin in these areas may thin out, leading to depression. While this condition can occur in people without diabetes, it’s more prevalent in those with the condition.
6. Dry and Itchy Patches
Dry, itchy skin is a common complaint among people with diabetes, especially on the feet and lower legs. High blood sugar can dehydrate the skin and impair sweat gland function, leading to dryness. Additionally, poor circulation and nerve damage can make the skin more prone to itching and irritation. If left unchecked, scratching can lead to infections, which are harder to heal in people with diabetes.
What Should You Do If You Notice These Signs?
If you’ve noticed any of these skin changes, don’t panic—but don’t ignore them either. Here are some steps you can take to address them and protect your health:
1. Consult a Healthcare Provider: A doctor can evaluate your symptoms, check your blood sugar levels, and determine if diabetes or another condition is the cause. They may recommend tests like a fasting blood sugar test or an A1C test to diagnose diabetes.
2. Manage Blood Sugar Levels: If you’ve already been diagnosed with diabetes, these skin changes might indicate that your condition isn’t well-controlled. Work with your doctor to adjust your treatment plan, which may include medication, diet changes, or increased physical activity.
3. Prioritize Skin Care: Keep your skin clean and moisturized to prevent dryness and infections. Use mild, fragrance-free soaps and lotions, and avoid scratching itchy areas. For those with diabetes, foot care is especially important—check your feet daily for cuts, blisters, or signs of infection.
4. Stay Hydrated: Drinking plenty of water can help combat dryness and support overall skin health. High blood sugar can lead to dehydration, so staying hydrated is key.
5. Monitor for Infections: People with diabetes are more prone to skin infections due to slower healing. If you notice redness, swelling, warmth, or pus around a skin lesion, seek medical attention promptly.
The Importance of Early Detection
Catching diabetes early—or managing it effectively—can make a huge difference in preventing complications. Skin changes are just one piece of the puzzle. Other common symptoms of diabetes include increased thirst, frequent urination, unexplained weight loss, fatigue, and blurred vision. If you’re experiencing a combination of these symptoms along with skin changes, it’s even more important to get checked out.

A Note of Inspiration for Rise & Inspire Readers
At Rise & Inspire, we believe in empowering you to take charge of your health and well-being. Your body often sends signals when something isn’t right, and learning to listen to those signals is a powerful act of self-care. Whether it’s a new patch of skin that looks unusual or a persistent itch that won’t go away, don’t hesitate to advocate for yourself and seek answers. You deserve to feel your best, and taking proactive steps can help you thrive.
If you or someone you know is living with diabetes, remember that you’re not alone. With the right support, education, and lifestyle changes, it’s possible to manage diabetes and live a full, vibrant life. Let’s keep inspiring each other to rise above challenges and prioritize our health!
Have you noticed any unusual skin changes lately? Share your experiences in the comments—we’d love to hear from you! As always, consult with a healthcare professional for personalized advice.
Stay healthy and inspired,
Rise & Inspire
Explore additional inspiration from the blog’s archive. | Others
Categories: Astrology & Numerology | Daily Prompts | Law | Motivational Blogs | Motivational Quotes | Others | Personal Development | Tech Insights | Wake-Up Calls
🌐 Home | Blog | About Us | Contact| Resources
📱 Follow us: @RiseNinspireHub
© 2025 Rise&Inspire. All Rights Reserved.
Word Count:1242